Page 1 of 1
On May 4, 2017, the IRS released Revenue Procedure 2017-37 setting dollar limitations for health savings accounts (HSAs) and high-deductible health plans (HDHPs) for 2018. HSAs are subject to annual aggregate contribution limits (i.e., employee and dependent contributions plus employer contributions). HSA participants age 55 or older can contribute additional catch-up contributions. Additionally, in order for an individual to contribute to an HSA, he or she must be enrolled in a HDHP meeting minimum deductible and maximum out-of-pocket thresholds. The contribution, deductible and out-of-pocket limitations for 2018 are shown in the table below (2017 limits are included for reference).
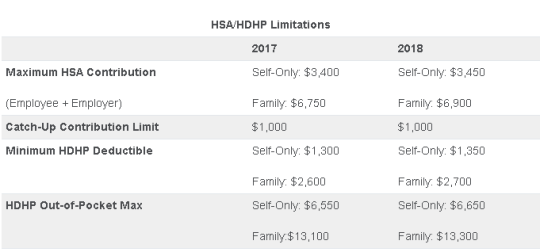
Note that the Affordable Care Act (ACA) also applies an out-of-pocket maximum on expenditures for essential health benefits. However, employers should keep in mind that the HDHP and ACA out-of-pocket maximums differ in a couple of respects. First, ACA out-of-pocket maximums are higher than the maximums for HDHPs. The ACA’s out-of-pocket maximum was identical to the HDHP maximum initially, but the Department of Health and Human Services (which sets the ACA limits) is required to use a different methodology than the IRS (which sets the HSA/HDHP limits) to determine annual inflation increases. That methodology has resulted in a higher out-of-pocket maximum under the ACA. The ACA out-of-pocket limitations for 2018 were announced are are $7350 for single and $14,700 for family.
Second, the ACA requires that the family out-of-pocket maximum include “embedded” self-only maximums on essential health benefits. For example, if an employee is enrolled in family coverage and one member of the family reaches the self-only out-of-pocket maximum on essential health benefits ($7,350 in 2018), that family member cannot incur additional cost-sharing expenses on essential health benefits, even if the family has not collectively reached the family maximum ($14,700 in 2018).
The HDHP rules do not have a similar rule, and therefore, one family member could incur expenses above the HDHP self-only out-of-pocket maximum ($6,650 in 2018). As an example, suppose that one family member incurs expenses of $10,000, $7,350 of which relate to essential health benefits, and no other family member has incurred expenses. That family member has not reached the HDHP maximum ($14,700 in 2018), which applies to all benefits, but has met the self-only embedded ACA maximum ($7,350 in 2018), which applies only to essential health benefits. Therefore, the family member cannot incur additional out-of-pocket expenses related to essential health benefits, but can incur out-of-pocket expenses on non-essential health benefits up to the HDHP family maximum (factoring in expenses incurred by other family members).
Employers should consider these limitations when planning for the 2018 benefit plan year and should review plan communications to ensure that the appropriate limits are reflected.
On March 1, 2016, the Department of Health and Human Services (HHS) announced the finalized 2017 health plan out-of-pocket (OOP) maximums. Applicable to non-grandfathered health plans, the OOP limits for plan years beginning on or after January 1, 2017 are $7,150 for single coverage and $14,300 for family coverage, up from $6,850 single/$13,700 family in 2016. The OOP maximum includes the annual deductible and any in-network cost-sharing obligations members have after the deductible is met. Premiums, pre-authorization penalties, and OOP expenses associated with out-of-network benefits are not required to be included in the OOP maximums.
In addition to the new OOP maximum limits, employers offering high deductible health plans need to be particularly mindful of the embedded OOP maximum requirement. Beginning in 2016, all non-grandfathered health plans, whether self-funded or fully insured, must apply an embedded OOP maximum to each individual enrolled in family coverage if the plan’s family OOP maximum exceeds the ACA’s OOP limit for self-only coverage ($7,150 for 2017). The ACA-required embedded OOP maximum is a new and often confusing concept for employers offering a high deductible health plan (HDHP). Prior to ACA, HDHPs commonly imposed one overall family OOP limit on family coverage (called an aggregate OOP) without an underlying individual OOP maximum for each covered family member. Now, HDHPs must comply with the IRS deductible and OOP parameters for self-only and family coverage in addition to ACA’s OOP embedded single limit requirement.
The IRS is expected to announce the 2017 HDHP deductible and OOP limits in May 2016.